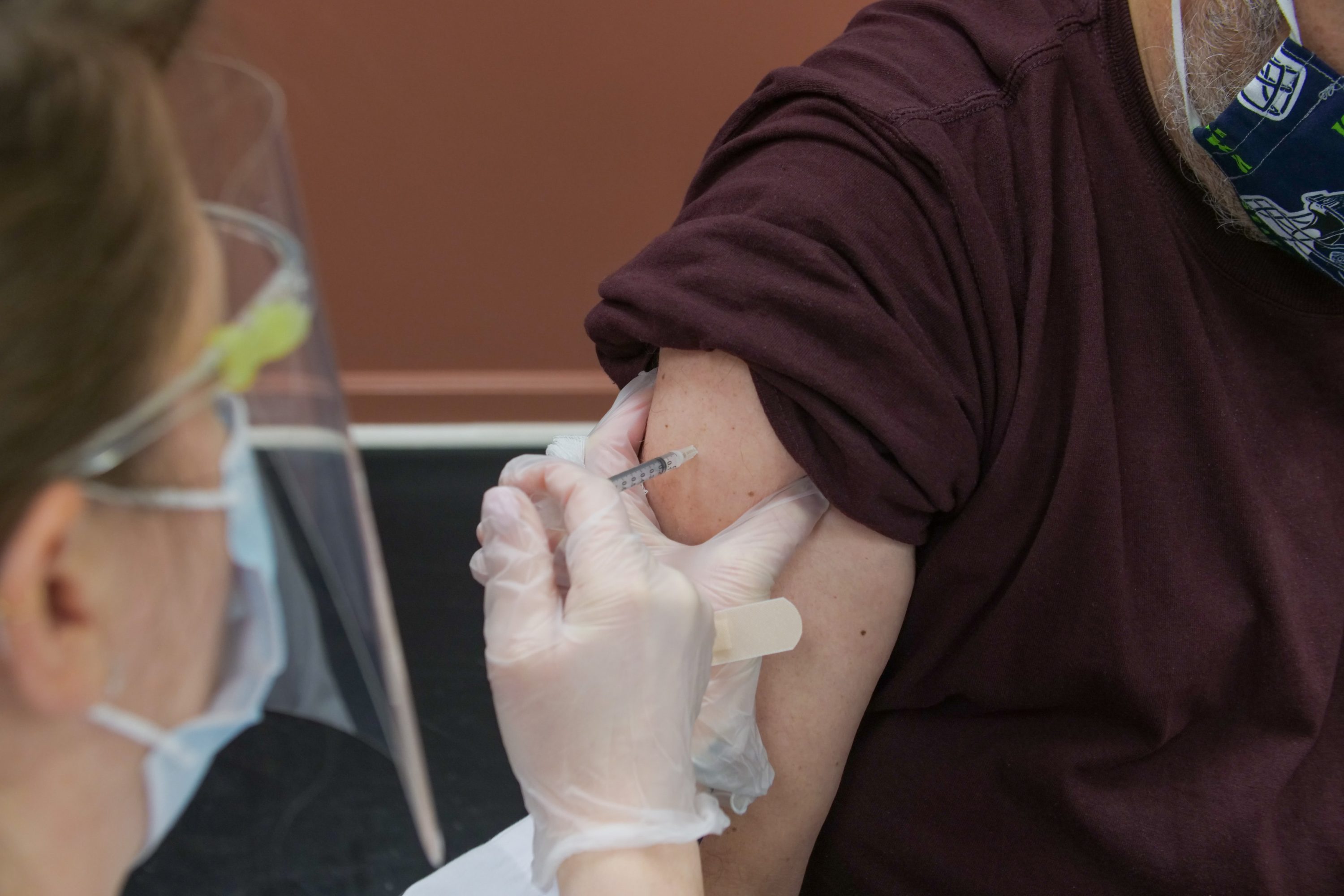
Although most consumers prefer to see their doctors in person, many are willing to continue using telehealth services that have increased in popularity during the COVID-19 pandemic, according to survey results released Wednesday.
The study by the Santa Monica-based think-tank the RAND Corporation — titled “Assessment of Patient Preferences for Telehealth in Post-COVID-19 Pandemic Health Care” — surveyed a representative sample of 2,080 Americans to ask about their experiences with telehealth and their preferences for in-person care or video visits in the future under different scenarios.
RAND researchers concluded that most consumers are less interested in using telehealth if the out-of-pocket cost is higher than for in-person care.
The study, considered the first to report on the willingness of the general U.S. population to pay for telehealth in a post-pandemic world, is published by the journal JAMA Network Open.
“Patients may like telehealth in certain circumstances such as when as when they need care for minor health issues,” said Zachary Predmore, the study’s lead author and an associate policy researcher at the nonprofit research organization. “But their willingness to use telehealth is very sensitive to costs. Patients may not perceive video visits to have the same value as in-person health care.”
RAND also found that people who preferred video visits were more sensitive to out-of-pocket costs than those who preferred in-person visits, as a $20 increase in cost was associated with more people switching from video visits to in-person care.
Use of telehealth has increased rapidly during the COVID-19 pandemic as health care providers offer telephone or video visits to reduce the potential for virus spread. A previous RAND survey found that 40% of Americans with a chronic health condition had used telehealth by the spring of 2020.
It is unclear how telehealth may be used within the U.S. health system after the pandemic, with early evidence suggesting that telehealth is decreasing as providers and patients resume in-person care. Federal programs such as Medicare and private insurers are weighing whether and how to pay for routine telehealth in the future.
“The results show that although many participants used telehealth for the first time during the pandemic out of necessity, their experiences were positive enough for them to use such services again,” Predmore said.
About 34% of participants did not see any role for video visits in their medical care. These people were generally older, had lower incomes, lived in more rural areas and had lower education levels, according to RAND.