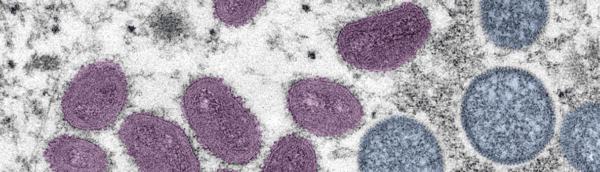
Now that California officially declared a state of emergency for monkeypox, residents may be left wondering what it is they can do to keep themselves from exposure. At the same time, details surrounding the virus aren’t as clear, with conflicting information coming out about confirmed cases, who it’s impacting, and how to stop it from impacting you.
With COVID fatigue draining the mental capacity of citizens, adding another virus to the disease watch might prove to be detrimental in slowing the spread of monkeypox. Unlike COVID, the mortality rate is one out of every 10 people, though precautions should still be taken due to the pain and discomfort level of the rash the virus causes.
White House Taking Action
Headway was made in regard to the virus at the beginning of August. The Biden administration named Robert Fenton, a vet emergency response official who is also the regional administrator for FEMA, as the White House’s monkeypox coordinator.
At the state level, Gov. Gavin Newsom declared a state of emergency for the virus just days after San Francisco made its city-wide declaration, having seen cases in the hundreds at the end of July.
Long Beach and Los Angeles County soon followed suit, with Biden putting the same designation over the entire country on Thursday. At time of publication, Riverside and San Bernardino Counties had yet to take the emergency step.
That’s because comparatively, the two counties have seen significantly fewer cases so far, currently only seeing 51 cases as of Friday.
Parsing The Numbers
What’s confusing, and maybe a bit misleading, is the language officials use surrounding infection figures. Health officials have been lumping probable cases with confirmed ones—the majority of which fall into the former category.
According to Riverside Public Health, a confirmed monkeypox case is one where a person has specifically tested positive for the monkeypox virus versus just testing positive for general Orthopoxvirus, which is the viral genus that monkeypox belongs to. If someone tests positive for the Orthopoxvirus genus, further testing is needed to confirm it’s the monkeypox strain.
Since monkeypox is a contact-driven virus, people might be more at risk of exposure now that the weather is warmer, schools will soon be back in session and businesses have largely reopened to regular operation.
Taking Precautions
While COVID precautions apply to a degree, monkeypox poses a different threat in its ease of transmission through bodily fluids, making it tantamount to pay close attention to contact with heavily trafficked surfaces like those in gyms and nail salons.
“Monkeypox is a particularly hardy virus … and it is known to be able to survive in linens, clothing and on environmental surfaces, particularly in dark and cool conditions, for up to two weeks or even longer,” Dr. Robert Bolan, LA’s LGBT Center’s medical director of research and education said during an interview with Yahoo.
“So, it’s very important, I think, to pay attention to environmental surfaces like gym surfaces and, you know, workout benches and mats — things that are completely porous … or partly porous” and to use disinfecting wipes or other household cleaners, which are effective when used correctly, he said.”
That said, the likelihood of contracting monkeypox is probably low.
Columbia Mailman School of Public Health Associate Professor of Medicine in epidemiology Dr. Jessica Justman also told Yahoo that the probability of catching the virus in the spaces is “unlikely” due to the lack of porosity of many of the surfaces because they’re easier to disinfect.
How does it spread and what are the symptoms?
Though unrelated to chickenpox, monkeypox in humans spreads in a similar fashion through close, skin-to-skin contact like kissing, hugging and intimate touching/intercourse.
Originally, the virus was mainly spread through a scratch or bite from an infected animal, but any type of exposure to monkeypox legions, rashes, scabs or fluids from someone with the virus can also cause infection. Those fluids include sweat, drool and respiratory discharges like mucus.
Coming into contact with fabric or other objects that an infected person has used could also lead to infection since the virus can survive up to 15 days on a surface. Mothers with the virus can pass it on to their fetus through their placenta, and someone could also get the virus by getting bitten, scratched, eating or using products that have been in contact with an infected animal.
While it’s unclear whether an asymptomatic person can spread the virus, a person with monkeypox is contagious from the moment they first experience symptoms until the rash has healed and new skin has formed. Infection, from initial symptoms to newly formed skin, generally lasts 2–4 weeks.
Flu-Like And Rash
Another similarity monkeypox has to COVID is in some of its initial symptoms, making it paramount to get tested if you’re experiencing them. They usually start within three weeks of exposure to the virus and if someone has flu-like symptoms, the rash will usually develop 1-4 days later.
Symptoms of monkeypox, according to the CDC, can include but are not limited to:
- Fever
- Respiratory symptoms like sore throat, nasal congestion, or cough
- Headache
- Muscle and/or backache
- Swollen lymph nodes
- Chills
- Exhaustion
Similar to aspects of certain sexually transmitted diseases, the monkeypox rash can appear anywhere on the genitals and the anus and will look like pimples, ingrown hairs or blisters that will go through several scabbing stages before healing. The painful and itchy rash isn’t localized to the genitals, as it can also appear on the face, chest, hand and feet. It is possible to get the rash without any of the other symptoms being present.
Troubling Rhetoric
In many of the confirmed monkeypox cases so far, men who have sex with other men have made up a majority of the infected persons, leading some of the public to believe that it only affects queer and gay men, and that it is an STI (sexually transmitted infection).
Officials are urging the public to recognize monkeypox, not as a “gay male disease,” but as one that can greatly affect anyone, since at least five children have tested positive for the virus in the United States (2 of which are in California, one of them in Long Beach).
“When public health bodies are saying we’re seeing men who have sex with men have monkeypox at a higher rate, people are hearing this as, ‘Oh, this is a gay disease’ or ‘This is another sexually transmitted disease.’ It’s getting conflated in people’s minds,” Dr. Stella Safo, an HIV primary care physician and founder of Just Equity For Health, told USA Today.
“There needs to be a really heavy-handed effort to make it very clear that while this group is affected more right now, we anticipate as this unfortunate virus becomes more prevalent in the community, that other groups will be impacted because of the way it spreads.”
The Southern California area has seen cases spread throughout the populace. It is not isolated to a specific community or group.
Remembering that monkeypox is a contact-based disease will help the public keep infection rates at bay, reminding them that thoroughly washing, sanitizing and disinfecting hands, surfaces and clothes is a necessary measure in slowing the spread.
Who Can Get The Vaccine And Where
There are currently two monkeypox vaccines on the market, JYNNEOS and ACAM2000, though JYNNEOS is the preferred one by health officials.
It’s a two-dose vaccine that takes 14 days after the second dose to fully protect the immune system. While ACAM2000 is an alternative, the single-dose vaccine takes four weeks to reach its potency in immune protection. It also has a higher likelihood of causing adverse side effects in those who receive it, so it is not recommended for those with other conditions or severely weakened immune systems.
Vaccine doses are limited throughout the country, as are test sites. Unlike COVID, where there are still somewhat accessible test sites and locations throughout the region, you must see your primary care provider if you feel you have symptoms or know that you have been directly exposed.
As of right now, you must register in both LA County and the City of Long Beach for a vaccination, and only if you meet these requirements:
- People who were exposed to someone with confirmed monkeypox and do not have symptoms.
- People who attended an event/venue where there was a high risk of exposure to someone with confirmed monkeypox.
- Gay or bisexual men and transgender persons who are on HIV pre-exposure prophylaxis (PrEP).
- Gay or bisexual men and transgender people who attended saunas, bathhouses, sex clubs, circuit parties or sex parties where they had anonymous sex or sex with multiple partners.
- Gay or bisexual men and transgender people with a diagnosis of gonorrhea or early syphilis within the past 12 months.
- Gay or bisexual men and transgender people 18 years of age and older who had multiple or anonymous sex partners in the last 14 days including engaging in survival and/or transactional sex (e.g., sex in exchange for shelter, food and other goods and needs).
- Residents who are immunocompromised, including those with advanced or uncontrolled HIV, may be at high risk for severe disease.
Pre-register for the monkeypox vaccine in Long Beach by going here and in LA County by going here.
Pasadena residents are only “invited” to receive the vaccine if they have a confirmed case. In Riverside, you must fill out a “vaccine interest form” before the county gives you information on when and where you can receive it.
San Bernardino County is only vaccinating exposed individuals and people with occupational risk at this time but those interested in the vaccine can fill out the “monkeypox vaccine interest form” on the county’s public health website.
Cervanté Pope can be reached at cpope@heymediagroup.com